Not Telehealth. Not Chat.
Structured Wound Intelligence.
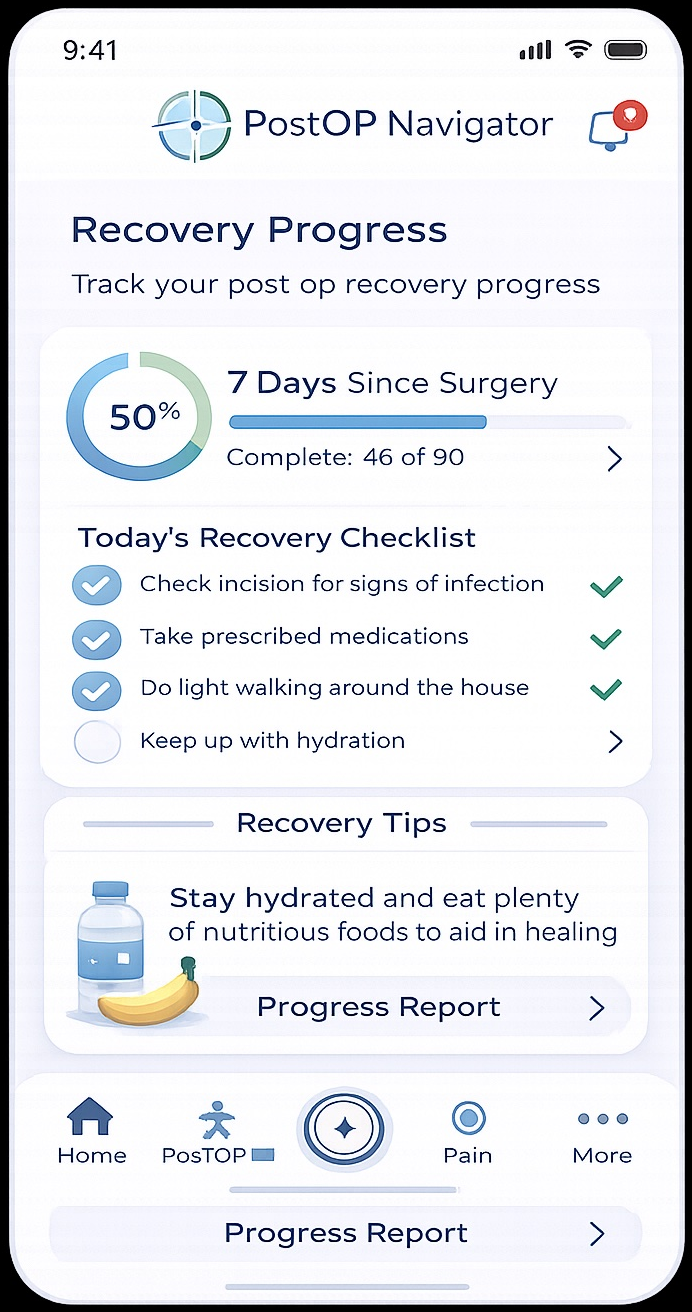
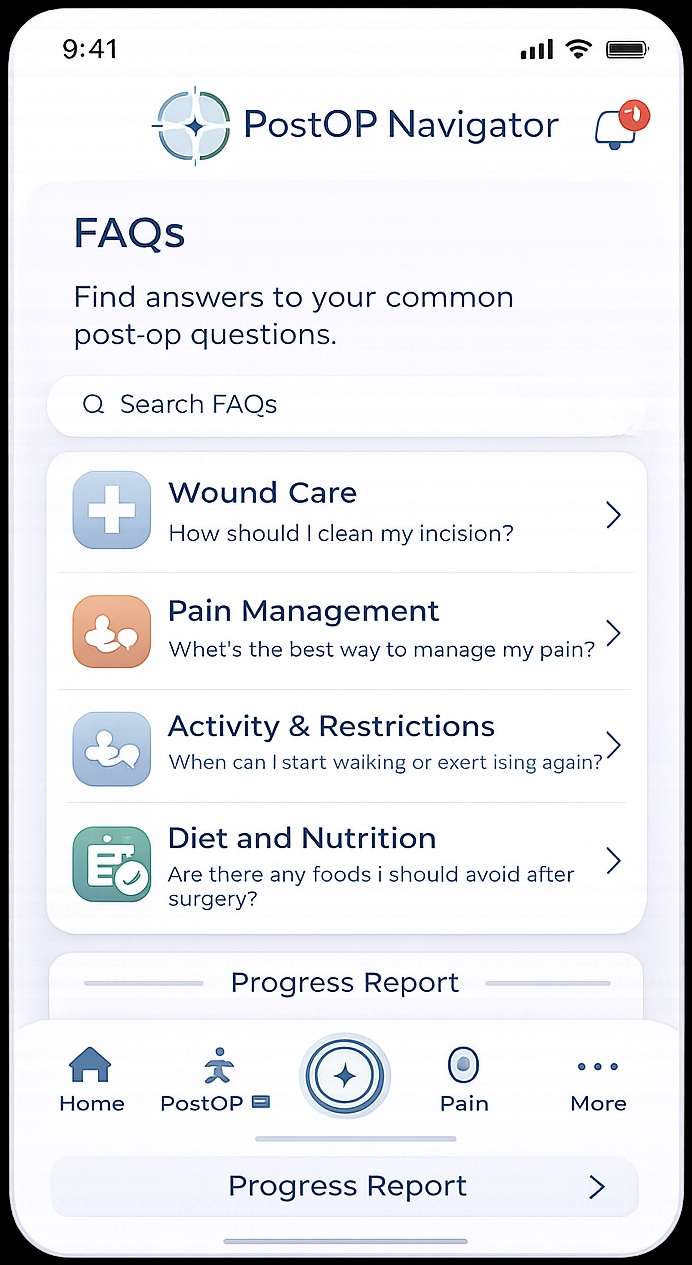
IncisionIQ applies CDC/NHSN wound surveillance criteria to every patient submission — with procedure context, healing phase calibration, and longitudinal change detection from day one.
Procedure-Aware Baseline Calibration
Healing expectations normalized per procedure, closure type, and post-op day.
Longitudinal Change Detection
Each patient's wound compared against their own prior images and expected recovery curve.
Surgeon Signature Learning
The model learns what normal healing looks like for each surgeon's specific technique.
NHSN-Grounded Wound Scoring
Terminology already embedded in hospital policy, payer contracts, and malpractice standards.
Human-in-the-Loop by Design
Every AI finding passes through a trained triage nurse — a structured input to clinical judgment.